Introduction
Acne is often described as a common condition, but the way it is treated can feel anything but straightforward. There are multiple options, ranging from pharmacy products and prescription medication to clinic-based procedures, and it is not always clear how these fit together. This can lead to uncertainty about where to start, when to change approach, or whether further treatment is necessary.
Understanding acne treatment matters because different approaches are designed for different stages and types of acne. What works well for mild breakouts may not be suitable for more persistent or inflammatory acne, and some treatments require careful supervision. Taking a structured, evidence-aware approach can help reduce unnecessary trial and error and lower the risk of irritation, delayed improvement, or scarring.
This guide sets out the main treatment options available in the UK, explaining how they work, when they are typically used, and what to expect from each stage. It also outlines how treatment pathways progress, from self-care through to specialist care, and where clinic-based treatments may fit alongside medical management. The aim is to provide clear, balanced information so you can decide what is relevant for your situation.
To begin, it helps to understand why acne is usually treated with a combination of approaches rather than a single solution.
LDM® Triple
LDM® Triple is a non-invasive ultrasound-based treatment used in aesthetic and dermatology clinics to support skin health, tissue regulation, and the Treatment of Acne-Prone or inflamed skin. This guide is for anyone trying to understand what it is, how it works, and whether it may be relevant to their skin concern.
- What LDM® Triple is, and how it differs from standard cosmetic ultrasound
- Which skin concerns it is commonly used for, including Acne and early ageing-related concerns
- What to consider around suitability, comfort, risks, pricing and provider choice
Visit Website
Understanding Acne Treatment: Why There Is No Single Solution
Acne treatment options are often described as a pathway rather than a single solution because the condition develops through several processes occurring simultaneously. Understanding this helps explain why combining treatments is usually more effective than relying on one product or approach.
What acne treatment is designed to target
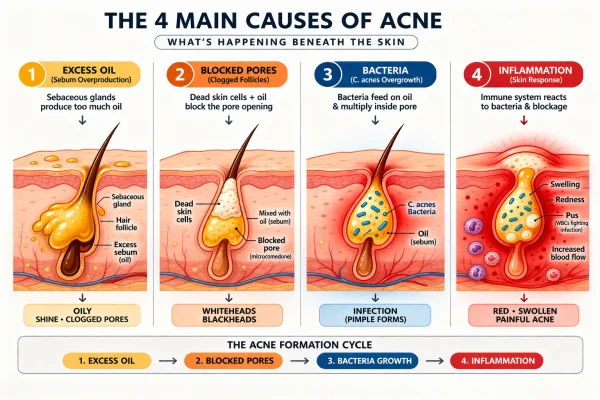
Most treatments focus on one or more of the underlying causes of acne:
-
Excess oil (sebum) production: Hormonal signals can increase oil output, particularly in adult and hormonal acne
-
Blocked pores: Dead skin cells can build up and prevent normal shedding within the follicle
-
Bacterial activity: Naturally occurring skin bacteria can contribute to inflammation when trapped in blocked pores
-
Inflammation: The immune response leads to redness, swelling, and more persistent lesions
Because these factors often occur together, treatments are typically combined to address them in parallel rather than sequentially.
Why does treatment take time to work
It is common for acne treatments to take several weeks before visible improvement:
-
Skin cell turnover takes around 4 to 6 weeks, which means blocked pores take time to clear
-
Early stages of treatment may bring underlying congestion to the surface
-
Clinical guidance in the UK usually recommends reviewing treatment at around 12 weeks
This timeline reflects how the skin functions rather than how effective a treatment is in the short term.
The role of consistency and realistic expectations
Consistency is one of the most important factors in successful acne management:
-
Treatments are usually applied to the entire affected area, not individual spots
-
Stopping and starting products can reduce effectiveness and increase irritation
-
Using multiple new products at once can make it difficult to identify what is helping or causing problems
A structured, steady approach is generally more effective than frequent changes based on short-term results.
In practice, acne treatment works best when it is approached as a coordinated plan rather than a single intervention. This becomes clearer when you look at how treatment pathways are structured in the UK.
Acne Treatment Pathways In The UK
From Self-Care to Specialist Care
Acne treatment options in the UK are usually structured in stages, moving from self-care through to specialist care if needed. This stepwise approach helps ensure treatment is appropriate to severity, while avoiding unnecessary medication or delays.

Starting with self-care and pharmacy treatments
For mild acne, treatment often begins with over-the-counter products and advice from a pharmacist:
-
Topical treatments such as benzoyl peroxide or azelaic acid are commonly recommended
-
Non-comedogenic skincare helps reduce pore blockage without overloading the skin
-
Pharmacist guidance can help you choose suitable products and avoid common mistakes
This stage is appropriate when acne is limited, not painful, and not causing scarring.
When GP-led prescription treatment is appropriate
If acne is persistent, spreading, or not responding to initial treatment, a GP may recommend prescription options:
-
Combination topical treatments (such as retinoids with benzoyl peroxide) are often first-line
-
Oral antibiotics may be introduced for more widespread or inflammatory acne
-
Treatment is usually reviewed after 12 weeks to assess response and tolerability
This stage aims to reduce inflammation and prevent progression, particularly when breakouts become more frequent or noticeable.
When referral to dermatology is recommended
Referral to a dermatologist-led service may be considered in specific situations:
-
Moderate to severe acne that has not responded to appropriate treatment
-
Risk of scarring, including deeper nodules or cysts
-
Significant psychological impact, such as low mood or reduced confidence
At this level, treatment may include isotretinoin, which requires closer monitoring and specialist oversight.
This structured pathway is designed to match treatment intensity to individual need. Understanding where you sit within it can help you make more informed decisions about when to continue, adjust, or escalate treatment.
Over-the-Counter And Skincare Treatments
For many people, acne treatment options begin with over-the-counter products and a consistent skincare routine. When used correctly, these approaches can be effective for mild acne and form the foundation of most treatment plans.
Key active ingredients and how they work
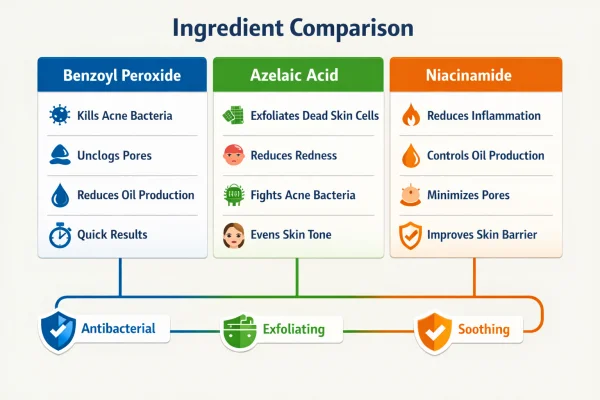
Over-the-counter treatments typically contain ingredients that target specific aspects of acne:
-
Benzoyl peroxide: helps reduce acne-causing bacteria and inflammation
-
Azelaic acid: supports pore clearance and can improve redness and uneven tone
-
Niacinamide: helps regulate oil production and supports the skin barrier
These ingredients are often available in gels, creams, or washes, and may be used alone or alongside prescription treatments.
Building a simple, effective routine
A straightforward routine is usually more effective than a complex one:
-
Cleanse twice daily using a gentle, non-alkaline cleanser
-
Apply treatment to the full affected area rather than individual spots
-
Moisturise to support the skin barrier and reduce irritation
-
Use sunscreen if treatments increase sensitivity to sunlight
Keeping the routine simple can reduce the risk of irritation and improve consistency over time.
Common mistakes that limit results
Some common habits can reduce the effectiveness of treatment:
-
Only treating visible spots, rather than the wider area where acne develops
-
Over-cleansing or over-exfoliating can disrupt the skin barrier
-
Stopping treatment too early, before results have had time to develop
-
Using multiple new products at once makes it difficult to assess what is working
Avoiding these patterns can improve outcomes without changing the treatment itself.
Over-the-counter treatments can be a useful starting point, but they are not always sufficient on their own. If improvement is limited, prescription options may be needed to address deeper or more persistent acne.
Prescription Treatments
What Your GP or Dermatologist May Recommend
When over-the-counter options are not enough, acne treatment options usually move to prescription therapies. These are selected based on severity, skin type, and previous response, and are often used in combination to improve outcomes.
Topical retinoids and combination treatments
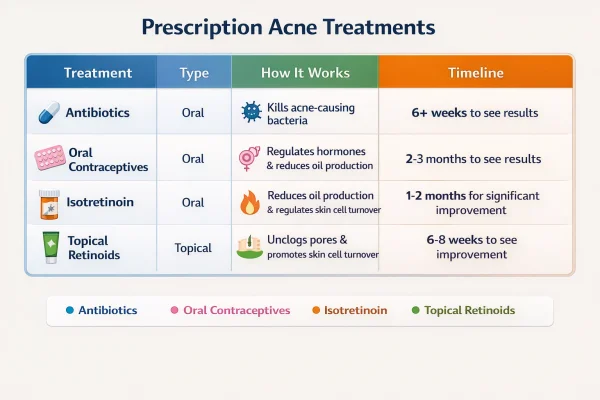
Topical treatments remain the foundation of most prescription plans:
-
Retinoids (such as adapalene or tretinoin) help normalise skin cell turnover and prevent blocked pores
-
Combination treatments often include benzoyl peroxide or a topical antibiotic to reduce inflammation and bacterial activity
-
These are typically applied to the full affected area, not just active spots
It is common for these treatments to cause temporary dryness or irritation, particularly in the first few weeks.
Oral antibiotics and when they are used
Oral antibiotics may be introduced when acne is more widespread or inflamed:
-
Common options include lymecycline or doxycycline
-
They are usually prescribed alongside a topical treatment rather than on their own
-
Courses are time-limited and reviewed regularly to reduce the risk of resistance
The aim is to reduce inflammation while longer-term treatments take effect.
Hormonal treatments for women
For women with acne linked to hormonal patterns, additional options may be considered:
These treatments are typically considered when breakouts follow a consistent pattern, such as around the jawline or menstrual cycle.
Isotretinoin for severe acne
Isotretinoin is usually reserved for more severe or treatment-resistant acne:
-
It works by significantly reducing oil production and inflammation
-
Treatment is prescribed and monitored by a dermatologist
-
Regular follow-up is required due to potential side effects
While it can be highly effective, it is introduced only after other appropriate treatments have been tried.
Prescription treatments are often an important step in controlling acne and preventing longer-term skin changes. They are most effective when used as part of a structured plan, with regular review and adjustment where needed.
Prescription Acne Treatments Comparison Table
Alongside medical care, some acne treatment options include professional procedures carried out in clinics. These are typically used to support skin recovery, reduce inflammation, or improve tolerance to other treatments, rather than replace prescription therapy.
Chemical peels and exfoliation treatments
Chemical peels use controlled exfoliation to support clearer skin:
-
Help remove dead skin cells that contribute to blocked pores
-
Can improve overall skin texture and tone over time
-
Often delivered as a course of treatments rather than a single session
Superficial peels are generally used for active acne, with strength and frequency tailored to skin sensitivity.
LED light therapy for acne
LED therapy uses specific wavelengths of light to support acne management:
-
Blue light targets acne-related bacteria
-
Red light supports the reduction of inflammation
-
Non-invasive and typically well tolerated
This treatment is often used as an adjunct, particularly for inflammatory acne or sensitive skin types.
Ultrasound-based treatments such as LDM Triple
LDM Triple is a clinic-based treatment that uses dual-frequency ultrasound:
-
Aims to support skin repair and regulate inflammatory processes
-
May be suitable for individuals with reactive or treatment-sensitive skin
-
Delivered as a series of sessions, often alongside other treatments
It is not a replacement for medical treatment in moderate to severe acne, but may support overall skin function.

Combining clinic treatments with medical care
Clinic-based treatments are usually most effective when integrated into a wider plan:
-
Can support the effects of topical or oral treatments
-
May help reduce irritation or improve skin tolerance
-
Require an appropriate assessment to ensure suitability
A personalised approach is important, as not all treatments are suitable for all skin types or acne patterns.
Professional treatments can play a supportive role in acne management when used appropriately. Understanding their place within a broader treatment plan helps set realistic expectations.
Choosing The Right Treatment Based On Acne Severity
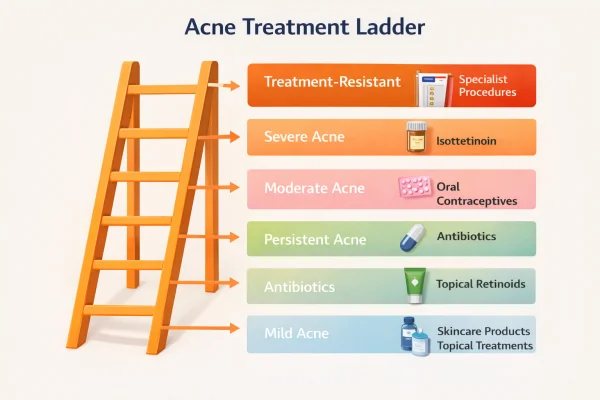
Acne treatment options are usually guided by severity, as this helps determine which approach is most likely to be effective. Matching treatment to severity reduces the risk of undertreatment or unnecessary escalation.
Mild acne treatment approach
Mild acne typically includes blackheads, whiteheads, and occasional inflamed spots:
-
Often managed with topical treatments such as benzoyl peroxide or retinoids
-
A consistent skincare routine plays a central role
-
Professional treatments may be considered if the response is limited
At this stage, treatment is usually focused on prevention and maintaining skin balance.
Moderate acne treatment approach
Moderate acne involves more frequent inflammation and a wider distribution of spots:
-
Combination topical treatments are commonly used
-
Oral antibiotics may be introduced to reduce inflammation
-
Regular review is important to assess progress and adjust treatment
This level often requires a more structured plan to prevent progression.
Severe acne and scarring risk
Severe acne may include nodules, cysts, or a higher risk of scarring:
-
Referral to a dermatologist-led service is usually recommended
-
Isotretinoin may be considered where other treatments have not been effective
-
Early intervention is important to reduce the likelihood of long-term skin changes
At this stage, treatment is more closely monitored and tailored to the individual.
Understanding severity helps clarify treatment decisions. It allows you to focus on appropriate options rather than trying multiple approaches without a clear structure.
Side Effects, Risks, And Limitations Of Acne Treatments
Most acne treatment options are safe when used appropriately, but it is important to understand potential side effects and limitations before starting. This helps set realistic expectations and supports informed decision-making.
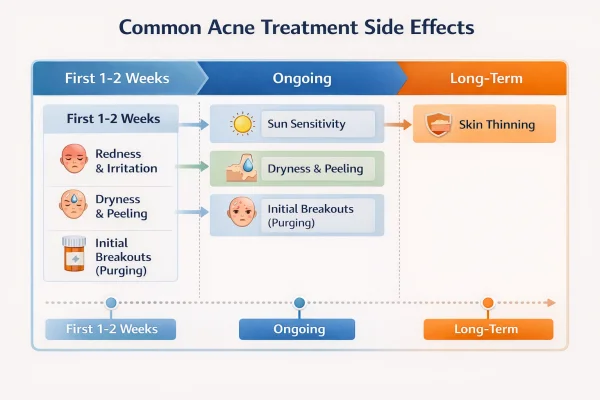
Common side effects of topical treatments
Topical treatments are widely used and generally well tolerated, but some initial reactions are expected:
-
Dryness and irritation, particularly with retinoids or benzoyl peroxide
-
Redness or peeling, especially in the early stages of use
-
Temporary worsening of acne, sometimes referred to as an initial flare
These effects are often managed by adjusting frequency or introducing products gradually.
Risks associated with oral medications
Oral treatments are used for more persistent or inflammatory acne and require closer supervision:
-
Antibiotics may cause digestive upset or sensitivity, and are usually prescribed for limited periods
-
Isotretinoin requires monitoring due to potential side effects, including skin dryness and changes in blood markers
-
Hormonal treatments may not be suitable for everyone and require an assessment of medical history
Regular follow-up helps ensure that treatment remains safe and appropriate.
Limitations and recurrence
Acne treatment can be effective, but there are some important limitations to be aware of:
-
Acne may recur after treatment, particularly if underlying triggers remain
-
Not all treatments work equally for every individual
-
Some treatments manage symptoms rather than providing a permanent resolution
Long-term management is often focused on maintaining results and preventing flare-ups.
Understanding potential side effects and limitations allows you to approach treatment with realistic expectations. This can make it easier to stay consistent and make informed adjustments when needed.









