Treatment for adult acne in the UK is usually guided by severity, skin sensitivity, and how your acne has responded to previous approaches. Most plans follow a stepwise structure, starting with topical treatments and progressing to prescription or clinic-based options if needed.
Over-the-counter and skincare-based approaches
For mild or early-stage adult acne, pharmacy and skincare treatments are often the starting point.
-
Benzoyl peroxide helps reduce bacteria and inflammation
-
Azelaic acid can improve both acne and pigmentation
-
Niacinamide supports oil regulation and skin barrier function
-
Non-comedogenic moisturisers and SPF help maintain skin balance
It is important to apply treatments consistently to affected areas, not just individual spots.
What this means for you:
These options can be effective for mild acne, but results take time and may be limited if deeper or hormonal factors are involved.
Prescription treatments
If acne is persistent or moderate in severity, a GP may recommend prescription treatments.
-
Topical retinoids help prevent blocked pores
-
Combination treatments (for example, retinoid with benzoyl peroxide or antibiotics) are commonly used
-
Oral antibiotics may be prescribed for inflammatory acne, usually for a limited duration
Treatment is typically reviewed after around 12 weeks to assess progress and next steps
What this means for you:
Prescription treatments are often more effective than over-the-counter options, but they require consistency and follow-up.
Hormonal treatments for women
Where acne is linked to hormonal patterns, specific treatments may be considered.
These treatments are usually considered when acne is persistent, cyclical, or not responding to standard approaches.
What this means for you:
Hormonal treatments can be helpful for the right patient group, but they require medical assessment and monitoring.
Specialist treatments for severe acne
For more severe or resistant acne, referral to a dermatologist may be recommended.
-
Isotretinoin is a specialist treatment used for severe acne or acne that has not responded to other therapies
-
Treatment is closely monitored due to potential side effects
-
Clear referral pathways exist within the UK healthcare system
What this means for you:
This option is usually considered when other treatments have not been effective, rather than as a first step.
Professional clinic treatments
Clinic-based treatments can support acne management, particularly alongside medical or skincare approaches.
-
Chemical peels help exfoliate and reduce blocked pores
-
LED light therapy may support inflammation reduction
-
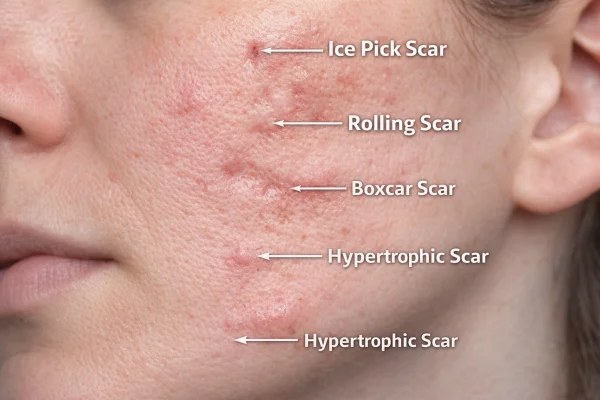
Microneedling is more commonly used for acne scarring rather than active acne
-
Ultrasound-based treatments such as LDM Triple are used in some clinics to support skin healing and reduce inflammation
These treatments vary in suitability depending on the severity of acne and skin type.
What this means for you:
Clinic treatments can complement a broader plan, but they are not usually a standalone solution for moderate-to-severe acne.
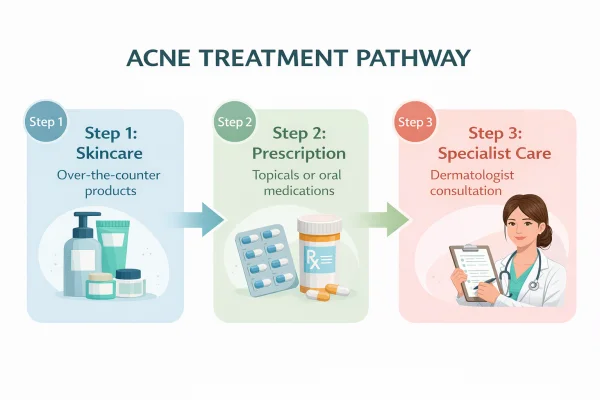
How treatment plans are typically structured
A structured approach helps avoid over-treatment or ineffective combinations.
-
Start with topical or skincare-based treatments for mild acne
-
Progress to prescription options if needed
-
Consider hormonal or specialist treatments for persistent cases
-
Use clinic treatments as supportive options where appropriate
Regular review is important to assess the response and adjust the plan.
Adult acne treatment in the UK is based on a stepwise, evidence-informed approach that balances effectiveness with safety. The most appropriate option depends on your acne severity, underlying causes, and how your skin responds over time.