Back acne rarely has a single cause. In most cases, several biological and environmental factors interact to create the conditions that lead to breakouts.
Understanding these triggers can help explain why bacne sometimes persists even when facial acne improves, and why management often involves a combination of skincare, lifestyle adjustments, and medical treatment when necessary.
Hormones and oil production
Hormones play an important role in regulating the skin’s oil production.
During certain stages of life, hormonal changes can increase the activity of the sebaceous glands, which produce sebum. When excess oil mixes with dead skin cells inside the hair follicle, the pore can become blocked, and acne may develop.
Situations where hormonal changes may contribute to bacne include:
-
Puberty, when androgen hormones increase oil production
-
Adult hormonal fluctuations, particularly in women during menstrual cycles
-
Hormonal conditions, such as polycystic ovary syndrome (PCOS)
-
Pregnancy or hormonal contraceptive changes
Hormonal acne often appears on the lower face and jawline, but the same hormonal influences can also affect the back and chest.
Sweat, exercise, and skin occlusion
Physical activity is important for overall health, but sweat and occlusion can contribute to back acne in some people.
Factors that may increase the likelihood of bacne include:
-
Sweat remaining on the skin for extended periods
-
Tight gym clothing that traps heat and moisture
-
Synthetic fabrics that reduce airflow
-
Pressure from backpacks or sports equipment
These conditions can create an environment where oil, sweat, and bacteria accumulate around the hair follicle.
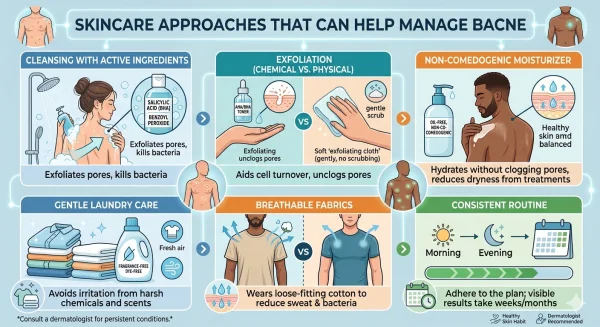
Practical habits that may help reduce this effect include showering after exercise, changing out of damp clothing promptly, and choosing breathable fabrics where possible.
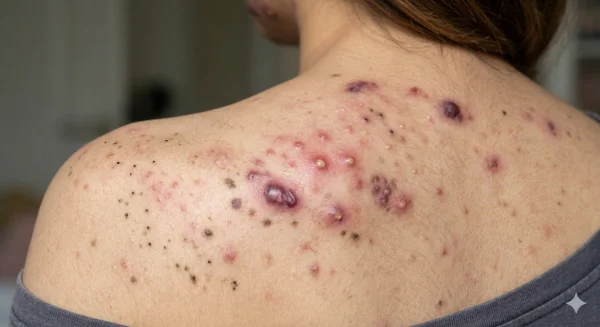
Skincare, hair products, and pore-blocking ingredients
Products applied to the hair and body can sometimes contribute to bacne, particularly when they leave residue on the skin.
Examples include:
When these products run down the back during washing or remain on the skin, they can clog pores in people prone to acne.
For this reason, many dermatology guidelines recommend choosing non-comedogenic products, which are formulated to reduce the likelihood of pore blockage.
Genetics and long-term acne patterns
Genetics can influence the likelihood that someone will develop acne and the severity of the acne.
Research has shown that:
-
Acne often runs in families
-
Individuals with a parental history of acne may develop earlier or more persistent acne.
-
Genetic factors can influence oil production, inflammation, and skin cell turnover.r
This does not mean acne is inevitable, but it can help explain why some people develop persistent bacne despite maintaining good skincare routines.
Back acne typically develops through a combination of hormonal activity, oil production, environmental triggers, and genetic susceptibility. Recognising these contributing factors can help guide practical changes and inform treatment decisions when breakouts persist.